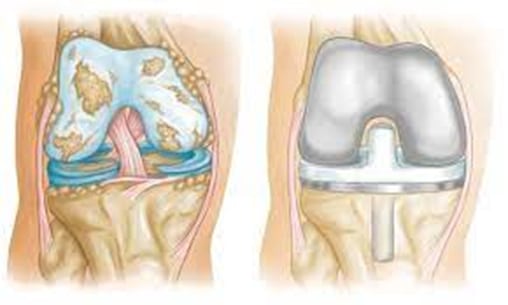
The first step when making the decision about knee replacement is to meet with your surgeon to see if you are a candidate for total knee replacement surgery. Your surgeon will take your medical history, perform a physical examination, and X-ray your knee. Even if the pain is significant, and the X-rays show advanced arthritis of the joint, the first line of treatment is nearly always non-operative. This includes weight loss if appropriate, an exercise regimen, medication, injections, or bracing. If the symptoms persist despite these measures, then you could consider surgery.
The decision to move forward with surgery is not always straight forward and usually involves a thoughtful conversation with yourself, your loved ones, and ultimately your surgeon. The final decision rests on you based on the pain and disability from the arthritis influencing your quality of life and daily activities. Those who decide to proceed with surgery commonly report that their symptoms keep them from participating in activities that are important to them like walking, taking stairs, working, sleeping, etc.) and that non-operative treatments have failed.
How long will it last?
A common reply to this question is that total joint replacement lasts 15-20 years. A more accurate way to think about longevity is via the annual failure rates. Most current data suggest that both hip and knee replacements have an annual failure rate between 0.5-1.0%. This means that if you have your total joint replaced today, you have a 90-95% chance that your joint will last 10 years, and an 80-85% that it will last 20 years. With improvements in technology, these numbers may improve.
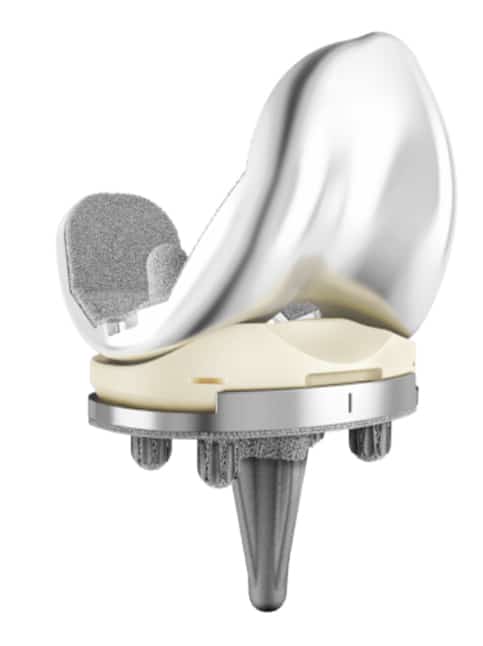
What types of implants will I get?
The orthopaedic implant industry has developed a number of innovative technologies in an effort to improve the outcomes of total joint replacement surgery. In recent years, these technologies have been marketed directly to patients, which has increased the awareness as well as confusion on what these different designs mean. The most important message is that while a certain manufacturer may claim that their design is better, almost all of the available registry data (large collections of data that track total joint surgery outcomes) show that there is no clear advantage to any of these designs when it comes to improving outcomes.
Will my surgeon use a computer, robot, or custom cutting guide in my surgery?
There are many studies attempting to evaluate these emerging technologies and their influence of the success of surgeries. Each of these technologies has a specific goal that has fueled its development (i.e. more accuracy in implant placement, more efficient or faster surgery, etc.). To date, there appears to be both pros and cons to each of these technologies without any clear advantages, but more research is required to determine what advantage, if any, these may offer. Despite a substantial amount of direct-to-consumer marketing, the best approach is to discuss this topic with your surgeon. You may want to know if they use one of these technologies, why they have chosen to do so, and what their experience has been in using it.
Dr. Shakir does use computer navigation for his knee replacements. He will use technology if necessary due to deformities or retained implants from previous surgeries. He is certified and credentialed to use computer navigation as well as Robotics during surgery.
Is knee surgery and recovery very painful?
Pain following total knee replacement has come a long way over the last 10-15 years with increased use of regional nerve blocks, spinal blocks, and various other modalities used for pain control. Total hip replacement is generally considered to be less painful than total knee replacement. Early range of motion and rapid rehabilitation protocols are also designed to reduce early stiffness and pain, making the procedure in general much less painful than in year’s past.
You may have relatively significant pain following the procedure for the first few weeks *this is normal and will continue to improve if you continue working hard with your physical therapist*.
You may have a more difficult or easier time than others- Remember everyone is unique and handles and perceives pain differently. Don’t compare your progress to others. Additionally, don’t compare one knee replacement to your second knee replacement- they are each unique!
What is minimally invasive surgery?
Minimally invasive surgery is a term that describes a combination of reducing the incision length and lessening tissue disruption beneath the incision. This includes cutting less muscle and detaching less tendon from bone. There have also been advancements in anesthesia and pain management during and after total knee replacement surgery. All of these practices allow you to feel better, have less pain, and regain function faster than in the recent past.
How big will my scar be?
The size of the incision can vary and depends on several factors that include the size of the patient, the complexity of the surgery, and surgeon preference. Most studies have shown that smaller incisions offer no improvement in pain or recovery and may actually worsen the surgeon’s ability to adequately perform the procedure.
Will I need general anesthesia?
While general anesthesia is a safe option, both hip and knee replacements can be performed under regional anesthesia. Choices for regional anesthesia include spinal anesthesia, epidural anesthesia, or one of a variety of peripheral nerve blocks.
Many surgeons and anesthesiologists prefer regional anesthesia because data shows it can reduce complications and improve your recovery experience with less pain, less nausea and less narcotic medicine required. Recently, peripheral nerve blocks have become more popular as an adjunct for pain control. For total knee replacement this can include an adductor canal block, which allows pain control without causing weakness of your muscles.
You should have a discussion regarding anesthesia and post-operative pain management with your anesthesia team prior to your surgery.
How long will I stay in the hospital?
You will likely stay in the hospital for one night depending on your rehabilitation protocol and how fast you progress with physical therapy. Some patients are going home same-day, considered “outpatient surgery”, if deemed safe at your appointment with your surgeon. This is highly dependent upon your condition before surgery, your age, and medical problems which can influence your rehabilitation. A safe discharge plan will be arranged for you by the orthopaedic team.
How long does it take to recover?
It can take up to three months for you to return to most activities, and likely six months to one year to fully recover to maximal strength and endurance following total knee replacement surgery. This depends on your condition before surgery, additional medical problems, and your expectations.
When can I shower?

Dr. Shakir uses a waterproof dressing that allow patients to shower the day after surgery. You can remove the dressing at seven to ten days after surgery. Once you remove the dressings, you still shouldn’t soak the wound until the incision is completely healed three to four weeks later. You will have steri-strips on underneath the bandage, those will stay on until they fall off.
When can I walk after surgery?
Most surgeons and hospitals today emphasize getting you out of bed quickly. Most people are walking with the assistance of a walker on the day after surgery and using a cane or nothing at all by two to three weeks.
When can I drive?
Most surgeons allow patients to drive at four to six weeks after surgery, and sometimes sooner if the operative leg is the left leg. There is some literature that states that your reaction time will not be back to normal prior to six weeks. You should not drive while on narcotics and should discuss returning to driving with your surgeon.
We typically allow you to drive if you are off the pain medications, off your walker and cane and we recommend practicing in a parking lot to make sure you are comfortable.
When can I return to work?
Returning to work is highly dependent on your general health, activity level and demands of your job. If you have a sedentary job, such as computer work, you can expect to return to work in four to six weeks. If you have a more demanding job that requires lifting, walking, or travel, you may need up to three months for full recovery.
What restrictions will I have after surgery?
Restrictions following total knee replacement surgery are generally few and should be discussed with your surgeon. After surgery, you will have some difficulty kneeling on the operative knee, which you will become less aware of with time, and you may experience clicking/popping sounds and sensation of a “mechanical knee”.
It may take you up to 12 – 18 months to fully recover!
Most people are able to return to usual activities and work but may have some difficulty performing heavy labor such as construction or farming. Most sporting activities are fine with the exception of running or jumping. Traveling should be not be affected by a joint replacement after the first four to six weeks when most surgeons advise against prolonged seated travel or flying due to increased risk of blood clot.
Will I need physical therapy, and if so, for how long?
Most people who have had a total knee replacement require outpatient physical therapy following surgery.
Dr. Shakir recommends outpatient physical therapy 3x week for 6 weeks as our gold standard.
A skilled therapist can accelerate the rehabilitation as well as make the process more efficient with the use of dedicated machines and therapeutic modalities. Depending on your condition before surgery, physical therapy is beneficial for up to three months and rarely longer. The amount of therapy needed depends upon your condition before surgery, motivation, and general health.
Are there complications to total knee replacement surgery?
- Total knee replacement surgery is primarily a pain-relieving procedure; however, it may not relieve all pain, and there is a possibility of residual stiffness and swelling.
- Although complications are relatively rare (1-2% of patients), patients may experience a complication in the postoperative period. These include very serious and possibly life- threatening complications such as heart attack, stroke, pulmonary embolism and kidney failure.
- Stiffness or loss of motion can also occur.
- Infection (1%) is one of the most debilitating complications and often requires prolonged antibiotics with several additional surgeries to rid the infection.
- A blood clot in the leg is also a relatively common complication requiring some type of blood thinner following surgery to reduce the incidence.
- The implants can also fail over time due to wear or loosening of the components, but this generally occurs many years after surgery.
Common questions
Constipation recommendations: Colace twice daily as a stool softener, along with miralax or dulcolax laxative. If no bowel movement after 3 days, advance to magnesium citrate or milk of magnesia (take as instructed on bottle). If no bowel movement by day 4, advanced to self-administered rectal suppository or enema. If by day 5, no bowel movement, we recommend going to emergency department. Additionally, warmed prune juice has been shown to be beneficial as well.
Sleep recommendations: For the first 6-12 weeks after a knee replacement, lack of sleep is a very common complaint as your body is trying to heal. Melatonin, Benadryl, Tylenol PM, CBD, and time seem to be the best methods. Unfortunately, patience is necessary to allow time for your body to heal.
Post-operative fever: It is common to run a low-grade fever post operatively. Be sure to be using your incentive spirometer, deep breathing, Tylenol 1000mg every 8 hours (unless told not to), and anti-inflammatory (unless told not to). Call our office if fever is >101.4.
Bruising/swelling post operatively: This is common after surgery, our recommendations include icing, resting, ACE wrap for compression, elevating and using conservative measures for comfort. This will continue to improve during your recovery. Make sure you are going to your physical therapy appointments. Make sure you are doing your ankle pumps, quad sets and glute squeezes 10x / hour daily and not getting up more than 10 minutes every hour you are awake for the first 2 weeks. Your physical therapist will transition you from walker to cane when they feel like you are stable and strong enough.
Post-operative bandage: This is typically removed 7-10 days post operatively with your physical therapist. If you do not have a scheduled appointment, you may remove yourself, leave the steri-strips in place. If you continue to have drainage, contact our office and we will guide you from there if you need to apply another bandage.